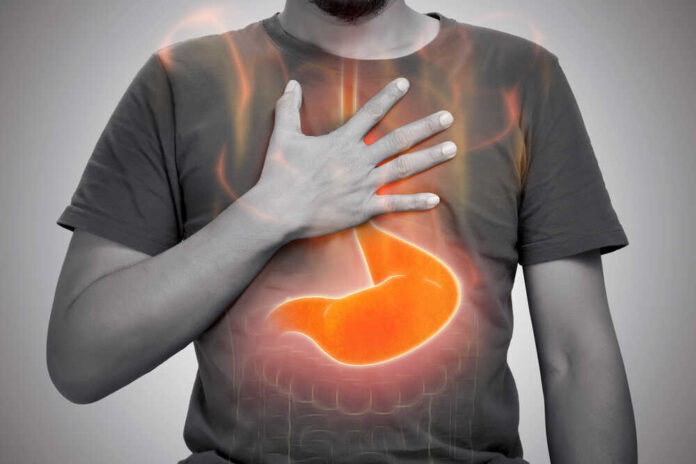
It’s never fun to feel as though you’ve swallowed a lump of burning coal, and if you’ve ever felt that tell-tale burn rising from your stomach to your chest after a meal, you’re not alone. Acid reflux—often called heartburn—affects millions of people daily. While occasional flare-ups are common, frequent reflux can be uncomfortable, disruptive, and, if ignored, potentially harmful over time. The good news? You don’t have to resign yourself to living with it. With some simple (and sometimes surprising) strategies, you can help tame the fire in your belly and reclaim your comfort.
- Rethink Your Mealtime Habits
It’s not just what you eat that matters—it’s how you eat.
- Go smaller, go smarter. Large meals stretch your stomach and put pressure on the lower esophageal sphincter (LES)—the valve that keeps stomach acid where it belongs. Aim for smaller, more frequent meals instead of giant portions.
- Slow down. Eating quickly often means swallowing air, chewing less, and overwhelming your digestive system. Try putting down your fork between bites, or timing your meal with a friend who eats more slowly.
- Sit upright. Lounging on the couch immediately after eating might sound cozy, but gravity is your friend. Stay upright for at least 2–3 hours after a meal to help prevent reflux.
- Identify Your Trigger Foods
Everyone has their personal “uh-oh” list when it comes to acid reflux. The most common culprits include:
- Spicy dishes (think chili, hot wings, or extra jalapeños)
- Acidic foods (tomatoes, citrus, vinegar-based dressings)
- Fatty or fried meals
- Chocolate, coffee, and caffeinated drinks
- Alcohol, particularly red wine and cocktails
That said, food sensitivities are highly individual. Keep a “reflux diary” for a couple of weeks—note what you eat, when symptoms flare, and how severe they are. You might discover that salsa doesn’t bother you but peppermint tea does, or that your reflux only shows up when you combine pizza with a beer.
- Mind Your Timing
Eating late at night can set you up for a rough bedtime. Try these timing tweaks:
- Finish dinner early. Stop eating at least three hours before lying down. That gives your stomach time to empty.
- Raise the head of your bed. If reflux still sneaks up on you at night, prop up your bed by 6–8 inches (pillows aren’t as effective as elevating the whole mattress). This allows gravity to help keep acid in place.
- Rethink Your Drinks
Beverages can be sneaky contributors to reflux.
- Limit alcohol and carbonated drinks. Bubbles expand the stomach, and alcohol relaxes the LES. A double whammy.
- Moderate your coffee intake. Some people can tolerate a small cup in the morning; others need to switch to herbal teas. Try experimenting with cold brew—it tends to be less acidic than hot coffee.
- Stay hydrated smartly. Water is generally safe, but avoid chugging large amounts all at once, especially during meals.
- Lifestyle Tweaks That Make a Difference
- Maintain a healthy weight. Extra abdominal pressure can push stomach contents upward. Even modest weight loss can ease reflux symptoms.
- Exercise smart. Movement is great for digestion, but avoid heavy lifting or intense workouts immediately after meals. Instead, try a light walk.
- Ditch tight clothing. Belts, shapewear, and snug waistbands can compress the stomach and worsen reflux.
- Stress Less, Digest Better
Believe it or not, your stress levels may influence reflux. Stress doesn’t directly cause acid reflux, but it can increase sensitivity to pain and alter digestive patterns.
- Mind-body practices like yoga, meditation, or simple deep breathing exercises can help.
- Make meals mindful. Eating while stressed or distracted often leads to overeating and poor digestion. Create a calm environment—even a few quiet minutes at the table can help.
- Over-the-Counter Helpers (With Caution)
Antacids (like Tums or Maalox) can provide quick relief by neutralizing stomach acid. H2 blockers (like famotidine) and proton pump inhibitors (PPIs, like omeprazole) reduce acid production more significantly. These can be effective tools, but:
- Don’t overuse. Long-term reliance on PPIs, for example, may affect nutrient absorption.
- Check with your doctor. Especially if symptoms are frequent (more than twice a week) or if you also experience trouble swallowing, unexplained weight loss, or chest pain.
- Know When to Seek Professional Help
Occasional heartburn is normal. But if acid reflux is frequent, severe, or affecting your sleep and daily life, it’s time to talk to a healthcare professional. Chronic reflux can damage the esophagus and increase the risk of complications like Barrett’s esophagus.
Managing acid reflux doesn’t mean giving up everything you love. It’s about balance, awareness, and small adjustments that add up. Think of it as an experiment: identify your triggers, tweak your lifestyle, and keep track of what works. Over time, you’ll build your own toolkit for keeping reflux at bay. In time, you can hopefully enjoy some pizza without fear of awakening the fire monster.
Copyright 2025, GoHealthier.com